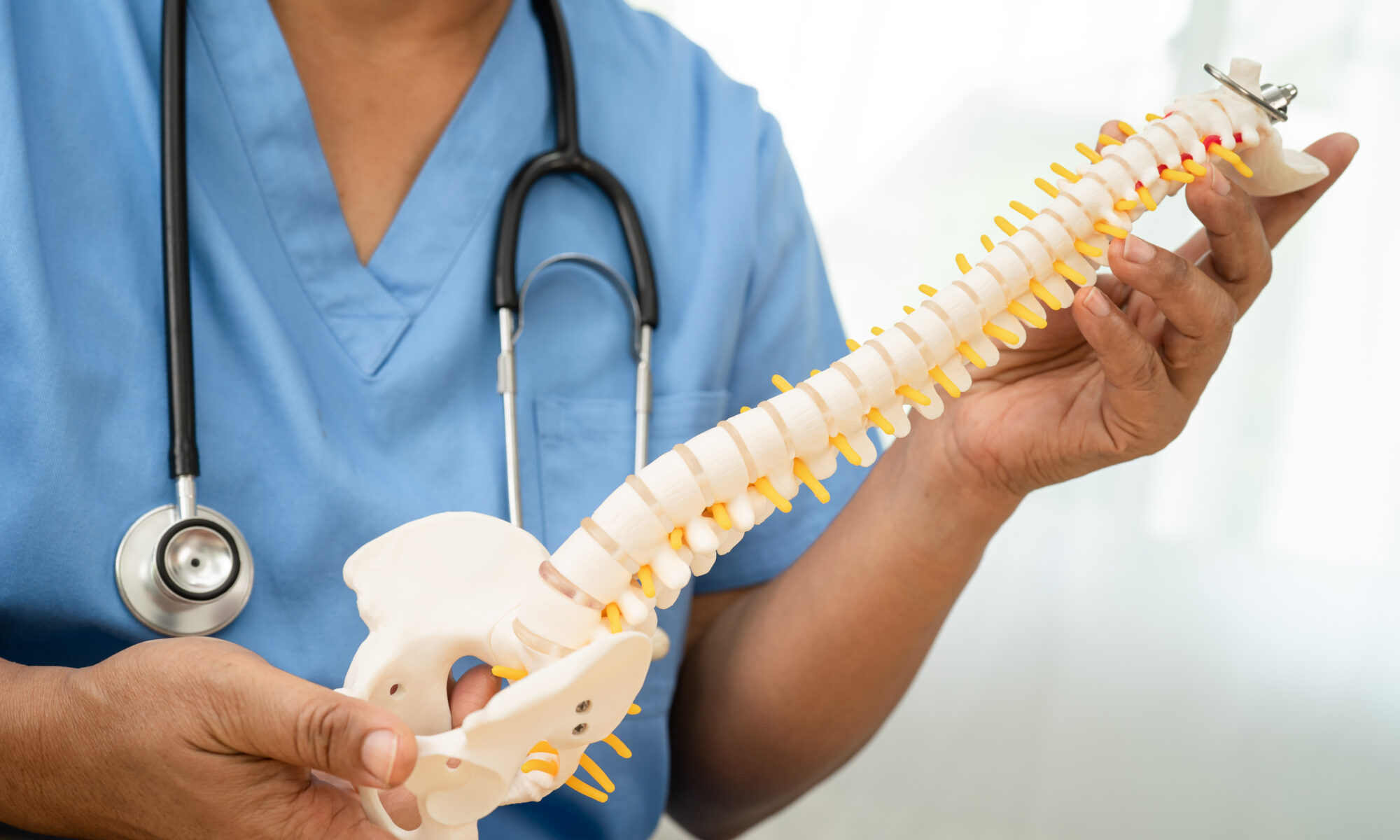
Disc-related back and leg pain can interfere with mobility, work, and overall quality of life, particularly when conservative treatment no longer provides relief. Back pain is a common symptom that often leads patients to consider endoscopic discectomy as a surgical option. Endoscopic discectomy benefits include targeted nerve decompression, limited disruption to surrounding tissue, and a shorter recovery period compared to traditional open spine surgery. This minimally invasive spine surgery technique offers an effective treatment option for carefully selected patients with disc herniation confirmed on imaging.
Endoscopic discectomy, also referred to as endoscopic diskectomy or endoscopic spinal surgery, uses minimally invasive techniques that allow surgeons to access the affected disc through a small incision using specialized instruments and direct visualization. These procedures address herniated discs that cause pain by relieving nerve compression. By limiting trauma to muscles and supporting structures, this approach preserves spinal stability while treating the source of symptoms.
Endoscopic discectomy is considered one of the least invasive surgical techniques available for treating spinal disc herniation.
Understanding endoscopic discectomy benefits, risks, and recovery expectations allows patients to make informed decisions about procedural care. Compared to traditional open or mini-open spine surgery, which requires longer incisions, endoscopic techniques rely on advanced technologies such as high-resolution cameras and real-time X-ray imaging to improve precision and reduce tissue disruption.
What is Endoscopic Spine Surgery?
Endoscopic spine surgery is a minimally invasive approach used to treat a range of spinal conditions. Instead of large incisions and extended hospital stays, surgeons access the spine through a small incision using an endoscope, which is a thin, flexible tube equipped with a camera and light. This technology allows direct visualization of the affected area and precise surgical intervention.
This approach reduces postoperative pain, limits tissue disruption, and supports a faster recovery. Many procedures are performed on an outpatient basis, allowing patients to return home the same day. By minimizing trauma to surrounding muscles and soft tissues, endoscopic spine surgery supports earlier return to daily activities and lowers the risk of complications compared to traditional open surgery.
Minimally Invasive Spine Surgery and Endoscopic Discectomy
Minimally invasive spine surgery focuses on treating spinal pathology while minimizing damage to surrounding tissues. Surgeons use smaller incisions, specialized instruments, and imaging guidance to reach the spine with precision. This approach reduces muscle disruption and often allows procedures to be performed in an outpatient setting.
Endoscopic discectomy represents a form of minimally invasive disc surgery that uses a camera-assisted view to identify and remove herniated disc material. The surgeon inserts a small metal tube and uses a tubular retractor to create a tunnel to the affected area, allowing direct visualization of the nerve root and disc. Real-time X-ray imaging (fluoroscopy) guides the precise placement of surgical instruments during the procedure. Lumbar discectomy is a specific type of endoscopic discectomy used to treat herniated discs in the lower back and typically results in reduced trauma and faster recovery compared to traditional open surgery.
ISSI incorporates endoscopic spine surgery into a broader treatment strategy when imaging and clinical findings confirm disc-related nerve compression. The procedure typically takes approximately 30 minutes, depending on anatomy and complexity.
What Lumbar Endoscopic Discectomy Treats
Lumbar endoscopic discectomy is a minimally invasive procedure designed to treat herniated discs in the lower back that compress spinal nerves. This compression often causes leg pain, numbness, or muscle weakness.
During the procedure, the surgeon makes a small skin incision and inserts an endoscope along with specialized surgical instruments to access the damaged disc. Using direct visualization, the surgeon removes only the portion of disc material compressing the nerve. Because this approach preserves surrounding tissues, patients often experience less postoperative pain and faster recovery compared to traditional spine surgery.
Lumbar endoscopic discectomy is commonly recommended when disc-related symptoms persist despite conservative treatment.
What Endoscopic Discectomy Treats and When It Is Used
Endoscopic discectomy treats disc herniation that compresses spinal nerves and leads to persistent symptoms. The procedure removes the portion of disc material pressing on the nerve root, reducing pain, numbness, and weakness.
Common indications for endoscopic discectomy include:
- Lumbar disc herniation causing leg pain
- Nerve root compression confirmed by MRI
- Symptoms that persist despite conservative care
- Functional limitations affecting daily activity
Endoscopic discectomy allows surgeons to avoid removing large amounts of bone or muscle to access the disc. Surgeons evaluate each case individually to ensure the procedure addresses the true source of symptoms rather than providing temporary relief.
Preparing for Endoscopic Spine Surgery
Proper preparation supports surgical safety and recovery. Assessing a patient’s overall health helps personalize surgical planning and establish realistic recovery expectations. Patients should review all medications and supplements with their healthcare provider, including nonprescription products. Some medications, such as blood thinners, may require temporary adjustment before surgery.
Preoperative imaging helps guide surgical planning and confirm the target disc level. Patients typically receive instructions regarding fasting, activity modification, and transportation home following the procedure. Smoking cessation is strongly recommended, as nicotine affects circulation and tissue healing.
To reduce infection risk, providers implement standard preoperative measures such as antibiotics and sterile technique. Following all preoperative instructions supports a smoother recovery process.
Endoscopic Discectomy Benefits Compared to Traditional Surgery
Endoscopic discectomy benefits extend beyond symptom relief and influence postoperative recovery and function. As a minimally invasive technique, endoscopic discectomy limits soft tissue disruption and preserves normal anatomy when appropriate, compared to traditional open spine surgery.
Key endoscopic discectomy benefits include:
- Smaller incision size
- Reduced muscle disruption
- Less postoperative pain in many patients
- Lower blood loss
- Faster return to daily activities for appropriate candidates
Surgical site infections may be significantly less common with endoscopic techniques compared to non-endoscopic methods. Continuous irrigation and small incisions help reduce infection risk and blood loss. Many patients require fewer pain medications after surgery compared to traditional approaches.
Endoscopic spine surgery allows surgeons to visualize the operative field through a small port, supporting precision and minimizing unnecessary tissue removal. Outcomes depend on diagnosis, disc size, nerve involvement, and overall health.
Conditions Treated With Endoscopic Discectomy
Endoscopic discectomy benefits patients with specific disc-related conditions, most commonly lumbar disc herniation. Back pain often leads patients to consider surgical treatment when disc material compresses a spinal nerve and causes radiating leg pain, numbness, or weakness.
This minimally invasive disc surgery approach relieves pressure on the nerve root while limiting removal of bone and muscle. Avoiding large incisions supports faster recovery and fewer postoperative limitations.
Appropriate patient selection remains critical. Endoscopic discectomy has demonstrated high success rates for pain relief and improved mobility in well-selected cases.
Risks of Endoscopic Discectomy
Although endoscopic discectomy benefits many patients, all surgical procedures carry risk. Potential risks include infection, bleeding, nerve irritation, nerve injury, spinal fluid leakage, incomplete symptom relief, or the need for additional treatment.
Risk varies depending on spinal level, patient health, and procedural complexity. ISSI specialists review imaging studies, medical history, and overall health before surgery to reduce complications. Surgeons use meticulous technique and imaging guidance to limit risk.
Clinical studies report patient satisfaction rates between 90 and 95 percent, with significant pain relief and functional improvement.
Managing Pain and Discomfort After Endoscopic Discectomy
Postoperative pain management plays an important role in recovery. While most patients experience less pain than with traditional spine surgery, some discomfort is expected during the healing process. Providers prescribe appropriate pain medication and may recommend ice or heat based on individual needs.
Gentle stretching, proper posture, and adherence to activity restrictions support healing. Follow-up appointments allow providers to assess recovery progress, adjust pain management strategies, and address concerns promptly.
Hospital Stay and Postoperative Care After Endoscopic Discectomy
Most patients are monitored in a recovery area immediately after surgery while anesthesia wears off. Many endoscopic discectomy procedures occur on an outpatient basis, allowing patients to return home the same day. Some individuals may require overnight observation depending on procedural or medical factors.
Postoperative care includes incision monitoring, activity restrictions, and pain management guidance. A back brace may be recommended for comfort or support. Most patients walk within hours after surgery and return to light activities or desk work within one to two weeks. Patients are encouraged to walk regularly to promote circulation and reduce the risk of blood clots.
Providers may recommend physical therapy to improve strength, mobility, and movement patterns. Follow-up visits allow the care team to adjust recovery plans as needed.
Endoscopic Discectomy Recovery Timeline
Endoscopic discectomy recovery often progresses faster than recovery after traditional surgery, although individual timelines vary.
Most patients:
- Walk shortly after surgery
- Resume light activity within days
- Return to desk work within one to two weeks
- Gradually increase activity over several weeks
Patients typically receive instructions for the first three weeks following surgery to protect the spine. Proper nutrition, including adequate vitamin intake, supports wound healing. Physical therapy may support long-term recovery and reduce recurrence risk.
Discectomy recovery time depends on disc involvement, nerve irritation, and adherence to postoperative guidance.
Long-Term Outcomes After Endoscopic Discectomy
Many patients experience significant improvement in pain and function following endoscopic discectomy. Mild stiffness or soreness may persist temporarily but usually improves with time and rehabilitation.
Long-term outcomes depend on diagnosis, surgical technique, and patient participation in recovery. In select cases, spinal fusion may be considered if additional stability is required. Maintaining proper body mechanics and addressing contributing factors supports durable results.
Who Is a Candidate for Endoscopic Discectomy
Not all disc conditions require surgery. An orthopedic surgeon evaluates whether endoscopic discectomy benefits outweigh risks based on imaging findings, symptom severity, response to conservative care, and overall health.
Candidates typically experience persistent nerve-related pain, functional limitations, and imaging-confirmed disc herniation. Nonsurgical treatments usually precede surgical consideration.
How ISSI Approaches Endoscopic Discectomy
At International Spine & Sports Institute, endoscopic discectomy fits within a comprehensive spine care approach. Specialists emphasize accurate diagnosis, patient education, and minimally invasive disc surgery when appropriate.
The procedure involves inserting an endoscope through an incision less than one centimeter, allowing surgeons to visualize and remove the herniated disc material using specialized graspers. ISSI develops individualized treatment plans based on patient goals, activity level, and recovery expectations.
When Discectomy Should Be Considered
Patients should consider surgical evaluation when disc-related symptoms:
- Persist despite conservative treatment
- Cause leg weakness or numbness
- Limit work, sports, or daily activities
- Progress over time
- Suggest spinal cord or nerve compression requiring timely intervention
Early evaluation helps determine whether endoscopic discectomy benefits apply to each case.
Life After Endoscopic Discectomy
Endoscopic discectomy benefits patients who require effective nerve decompression without prolonged recovery. As an outpatient procedure, many patients return home the same day and resume daily activities sooner than with traditional surgery.
With appropriate evaluation, careful patient selection, and experienced surgical care, many individuals regain mobility and functional independence. Maintaining spinal health after surgery supports optimal long-term outcomes.
Additional Considerations for Long-Term Recovery
Successful outcomes extend beyond the operating room. Physical therapy supports muscle strength, flexibility, and spinal stability. Providers design individualized rehabilitation programs to reduce recurrence risk and support functional recovery.
Understanding potential risks, adhering to postoperative instructions, and maintaining open communication with the care team contribute to positive outcomes. With informed decision-making and consistent follow-up, patients can achieve meaningful relief and long-term improvement after endoscopic discectomy.